Article Highlights
-
The NICHD-funded MFMU Network launched a large study of COVID-19 in pregnancy and has preliminary results.
-
Most pregnant women who get COVID-19 do well, but the disease raises the risk of pregnancy problems.
-
Read one woman’s story about getting COVID-19 while pregnant.
Andrea Castellon and her husband were over the moon in September 2020 when they learned she was expecting a baby. But then they realized that Andrea would be going through pregnancy, labor and delivery, and a hospital stay during the COVID-19 pandemic. The family was being careful to stay safe, but they knew how dangerous the disease could be.
Despite their precautions, in February 2021, the couple’s 2-year-old was diagnosed with COVID-19.
“When our daughter woke up one morning with a fever and then tested positive for COVID-19, I knew that it was only a matter of days before I got it,” Andrea recalled.
Her daughter recovered quickly, but, sure enough, Andrea started to show symptoms: fever, aching muscles, headache, dry cough, racing pulse, no sense of smell. Being sick with COVID-19 was bad, but she was extra worried because of the pregnancy.
“It was scary,” said Andrea. “Many people were getting sick and dying. Now I had it.” Andrea’s own father had died of COVID-19 in Ecuador just two weeks before she got sick.
Making things even worse were all the unknowns.
“No one — not even my midwife or doctor — knew how COVID-19 affects pregnancy,” Andrea said. “We were really stressed out and wished we had reliable information about the risks for pregnant women and their babies.”
A study supported by the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) is collecting the information that pregnant people and their doctors need. The Gestational Research Assessments for COVID-19 (GRAVID) study is studying the effects of SARS-CoV-2, the virus that causes COVID-19, during and right after pregnancy.
“No one — not even my midwife or doctor — knew how COVID-19 affects pregnancy. We were really stressed out and wished we had reliable information about the risks for pregnant women and their babies.” —Andrea Castellon

Andrea and Julio Castellon can breathe easier now that Andrea has recovered from COVID-19. They look forward to the birth of their son in the spring of 2021. Photo courtesy of the Castellons.

Andrea and Julio Castellon can breathe easier now that Andrea has recovered from COVID-19. They look forward to the birth of their son in the spring of 2021. Photo courtesy of the Castellons.
Power in numbers
How many pregnant women get COVID-19? Are some women at greater risk of getting severe disease while pregnant? Is it OK to skip office visits for prenatal care? Can the virus affect the fetus?
The GRAVID study aims to answer these questions and more. Torri Metz, M.D., M.S., of University of Utah Health, Salt Lake City, and Rebecca Clifton, Ph.D., of the Milken Institute School of Public Health at George Washington University, Washington, D.C., are leading the study.
“When we realized that we didn’t really know how COVID-19 affects pregnant people and newborns, we thought about harnessing the power of the Maternal-Fetal Medicine Units (MFMU) Network to conduct a study across the United States,” Dr. Metz said. MFMU Network studies have been improving pregnancy care since the network’s founding in 1986.
Dr. Metz is one of the MFMU Network’s 12 principal investigators, and Dr. Clifton runs the network’s data coordinating center. With long-standing NICHD support, the MFMU Network already had systems and scientists in place for doing large studies. It didn’t take the network’s researchers much time at all to launch the GRAVID study.
For the main GRAVID study, MFMU Network researchers are analyzing medical records of more than 25,000 women who gave birth in 2019 and 2020 at any of the MFMU Network hospitals. The study includes every woman who tested positive for SARS-CoV-2, plus a comparison group of randomly selected people who tested negative.
The scientists are studying COVID-19 severity in pregnant people and tracking numbers of pregnancy complications and C-sections. In addition, the researchers are evaluating whether giving birth during the pandemic, regardless of COVID-19 status, is linked with pregnancy-related problems or death. They also check whether newborns test positive for the virus.
Dr. Metz anticipates that results of the main GRAVID study will be published sometime in 2021.

How COVID-19 Affects Pregnancy
Should you get the vaccine during pregnancy? Does the vaccine cause infertility? NIH research is helping to answer these questions and more.
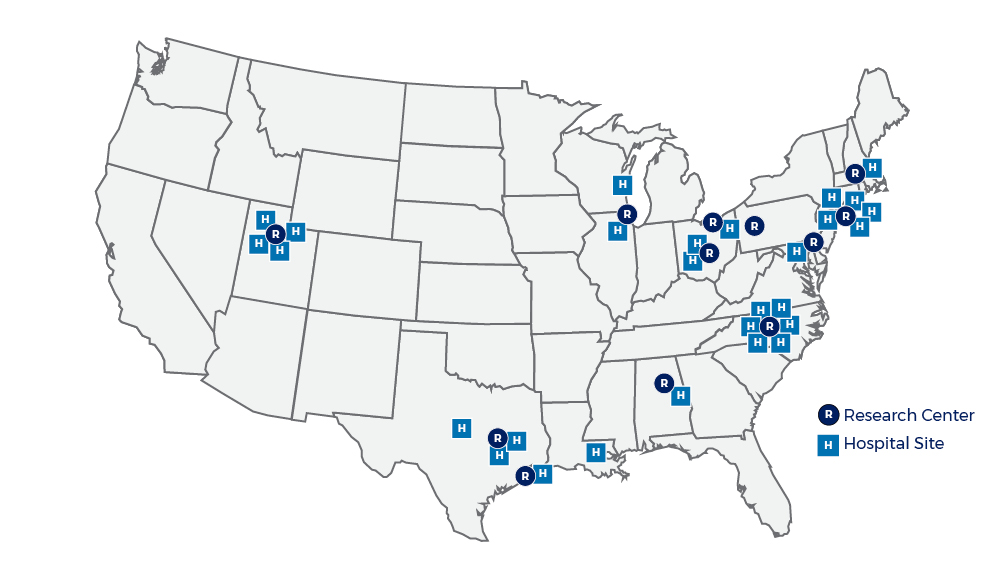
The MFMU Network includes 36 hospital sites affiliated with 12 research centers. Map courtesy of Rebecca Clifton, Ph.D., Milken Institute School of Public Health at George Washington University.

The MFMU Network includes 36 hospital sites affiliated with 12 research centers. Map courtesy of Rebecca Clifton, Ph.D., Milken Institute School of Public Health at George Washington University.
What have scientists learned so far?
To get some quick answers about the effects of SARS-CoV-2 on pregnancy, Dr. Metz led a subproject focusing on 1,200 pregnant women who delivered at hospitals that participate in the MFMU Network and tested positive for COVID-19 between March 1 and July 31, 2020.
“We felt it was very important to do this smaller study so we could get data into the hands of pregnant people and their doctors quickly,” Dr. Metz said.
The subproject results were published in the journal Obstetrics & Gynecology in April 2021.
“The good news is that nearly half of the 1,200 patients with positive COVID-19 tests never had any symptoms, and 40% had only mild or moderate symptoms,” Dr. Metz said. “We also learned that patients who had milder illness did not have a higher risk of pregnancy complications. Plus, we found that the virus does not often go from the mother to the fetus.”
Unfortunately, about 12% of the women experienced serious symptoms of COVID-19, and four women (0.3% of the group) died. Older women tended to be sicker, as did women who had a higher body mass index or other medical conditions, such as asthma or high blood pressure. Women with severe COVID-19 had a high risk of pregnancy-related problems, such as preeclampsia and eclampsia and preterm birth. Infants born to women with serious illness were more likely to be small and in need of intensive care. Data from the Centers for Disease Control and Prevention show that pregnant patients are more likely to need treatment in an intensive care unit and to need a breathing tube when they get SARS-CoV-2 than women who are not pregnant.
The main lesson of the subproject is clear: Pregnant women need to be careful to avoid getting COVID-19.
"The findings of the GRAVID study have the potential to shape pregnancy care now and during future pandemics." —Diana W. Bianchi, M.D.
Treating COVID-19 during pregnancy: A big question mark
Andrea learned firsthand about the uncertainties of treating COVID-19 in pregnant women when she developed serious illness that put her in the hospital for four days.
“My lungs weren’t working well because I had pneumonia,” Andrea said. “I needed antibiotics and steroid treatments.” She did not need a ventilator, but she did need oxygen therapy for a month. She and her doctor discussed COVID-19 treatments such as remdesivir and immune plasma, but there was little information about using them for pregnant patients.
The GRAVID researchers are collecting data on the safety of COVID-19 treatments in pregnancy. The study is also addressing questions about changes in medical practice due to the pandemic. Andrea is not in the study, but the results from GRAVID will help people like her.
“Early in the pandemic, many doctors reduced office visits and relied on telehealth visits to reduce the likelihood of exposure,” Dr. Metz said. “The GRAVID study is collecting data to learn whether these changes are affecting pregnancy outcomes.”
Having fewer in-person visits for prenatal care was a source of stress for Andrea and her husband.
“Because of the pandemic, office visits were limited,” Andrea said. “Then, after I had COVID-19, we really wanted to know that the baby was OK after I went home from the hospital, but I couldn’t go to medical facilities for a while.”
The GRAVID study results are likely to factor into decisions about prenatal care during pandemics, according to NICHD Director Diana W. Bianchi, M.D.
“The findings of the GRAVID study have the potential to shape pregnancy care now and during future pandemics,” Dr. Bianchi said. “For some women, severe COVID-19 can lead to serious complications for moms and babies. By identifying factors that may increase risk for severe disease, we have opportunities to identify high-risk pregnancies and prevent complications.”
Follow-up health checks have shown that Andrea’s pregnancy seems to be unaffected by COVID-19.
“I hope having some answers from research can help other families avoid the stress and uncertainties we faced,” Andrea said.
Sources
Centers for Disease Control and Prevention. (2021, March 12). Risk for COVID-19 infection, hospitalization, and death by race/ethnicity. Retrieved April 16, 2021, from https://www.cdc.gov/coronavirus/2019-ncov/covid-data/investigations-discovery/hospitalization-death-by-race-ethnicity.html
Metz, T. D., Clifton, R. G., Hughes, B. L., Sandoval, G., Saade, G. R., Grobman, W. A., Manuck, T. A., Miodovnik, M., Sowles, A., Clark, K., Gyamfi-Bannerman, C., Mendez-Figueroa, H., Sehdev, H. M., Rouse, D. J., Tita, A., Bailit, J., Costantine, M. M., Simhan, H. N., Macones, G. A., & Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) Maternal-Fetal Medicine Units (MFMU) Network (2021). Disease severity and perinatal outcomes of pregnant patients with coronavirus disease 2019 (COVID-19). Obstetrics & Gynecology, 137(4), 571–580. https://doi.org/10.1097/AOG.0000000000004339
Rasmussen, S. A., Kelley, C. F., Horton, J. P., & Jamieson, D. J. (2021). Coronavirus disease 2019 (COVID-19) vaccines and pregnancy: What obstetricians need to know. Obstetrics & Gynecology, 137(3), 408–414. https://doi.org/10.1097/AOG.0000000000004290
George Washington University. (2020). Maternal-Fetal Medicine Units Network. Retrieved April 12, 2021, from https://mfmunetwork.bsc.gwu.edu/PublicBSC/MFMU/MFMUPublic/
Wastnedge, E., Reynolds, R. M., van Boeckel, S. R., Stock, S. J., Denison, F. C., Maybin, J. A., & Critchley, H. (2021). Pregnancy and COVID-19. Physiological Reviews, 101(1), 303–318. https://doi.org/10.1152/physrev.00024.2020
Zambrano, L. D., Ellington, S., Strid, P., Galang, R. R., Oduyebo, T., Tong, V. T., Woodworth, K. R., Nahabedian, J. F., 3rd, Azziz-Baumgartner, E., Gilboa, S. M., Meaney-Delman, D., & CDC COVID-19 Response Pregnancy and Infant Linked Outcomes Team (2020). Update: Characteristics of symptomatic women of reproductive age with laboratory-confirmed SARS-CoV-2 infection by pregnancy status — United States, January 22–October 3, 2020. MMWR Morbidity and Mortality Weekly Report, 69(44), 1641–1647. https://doi.org/10.15585/mmwr.mm6944e3
 An official website of the United States government
An official website of the United States government