Article Highlights
-
Many clinical trials need to increase enrollment of people who are Black or African American, American Indian, Alaska Native, or Hispanic or Latino/a.
-
For COVID-19 vaccine clinical trials, researchers were able to create more diverse trials by building upon strong relationships established through decades of HIV research.
-
Because of that history of community engagement, 47% of COVID-19 vaccine clinical trial participants recruited by one HIV research network were Black, Indigenous, or people of color (BIPOC).
The core components of the COVID-19 vaccines were developed shortly after the SARS-CoV-2 genome was sequenced in mid-January of 2020. But finding out whether those vaccines were safe and effective required clinical trials involving tens of thousands of volunteers.
The impacts of the COVID-19 pandemic fell disproportionately on Black, Indigenous, and people of color (BIPOC), and the volunteers needed to represent the diversity of the United States to ensure that vaccines worked for those most affected. That’s why Michele Andrasik, Ph.D., director of social and behavioral sciences and community engagement at the HIV Vaccine Trials Network (HVTN), picked up the phone.
HVTN is one of four research networks funded by the National Institute of Allergy and Infectious Diseases (NIAID), three of which focus primarily on HIV. These networks were called on to recruit participants and run clinical trials of COVID-19 vaccines, and together they formed the new COVID-19 Prevention Network (CoVPN).
“Nationally, I called about 50 of our partners, plus more partners overseas,” says Andrasik. She talked with representatives of underrepresented groups “to really to get a sense of what people were seeing in their communities and what they felt the major needs were in terms of engaging communities in this work.”
During their decades of work on HIV, the three HIV/AIDS clinical trial networks and their sites have built strong relationships with Black and African American communities and Hispanic and Latino/a communities, which has laid a critical foundation for the networks as they pivoted to work as part of CoVPN. Andrasik and her colleagues understood how the COVID-19 pandemic would disproportionately impact these groups before that impact was more widely known, and CoVPN was able to swing into action. While some vaccine testing sites struggled to enroll non-White participants, the CoVPN sites that were part of HVTN and the other HIV/AIDS networks were able to enroll many people of color and ensure that trials for COVID-19 vaccines would include people who represent the diversity of the U.S. population.
“We want to make a vaccine that works for all of us,” says Andrasik. “We need to make sure that those who are most impacted are included in the trials.”

An HVTN site recruiter (left) speaks to people in a busy public setting in a Latino neighborhood. Photo courtesy of HIV Vaccine Trials Network.

An HVTN site recruiter (left) speaks to people in a busy public setting in a Latino neighborhood. Photo courtesy of HIV Vaccine Trials Network.
A history of community engagement
Founded with a NIAID grant in 1999, HVTN has spent more than two decades leading HIV vaccine research and ensuring that different studies produce results that can be compared with one another.
HIV/AIDS research has uniquely close ties with community groups because of the disease’s history. When HIV/AIDS first emerged — and for decades afterward — people with it experienced severe stigma. The information that was publicly available about the condition didn’t match the varied experiences of the people living with the disease. Community activist groups like ACT UP fought hard for recognition and research to better understand HIV/AIDS.
“Community has really always been at the center of HIV,” says Andrasik. “Anyone who is doing HIV research recognizes the importance of community engagement and makes sure that community is central.”
Every HVTN site has a community advisory board to ensure that local voices are included at every step of the clinical trial, from design to recruitment to implementation. Some community advisory board members have participated with HVTN sites for years or decades, says Andrasik.
Ensuring diverse COVID-19 vaccine trials
Compared with the U.S. population, the people in the average clinical trial are more likely to be White and less likely to be Black or African American, American Indian, Alaska Native, or Hispanic or Latino. Andrasik and her colleagues in CoVPN knew that BIPOC people needed to be present in clinical trials in the same percentages as in the U.S. population — or in even higher percentages.
As COVID-19 vaccines approached the clinical trial stage, more than 20 HVTN sites in the United States — including four sites at historically Black medical colleges and three sites on or close to Tribal Nations — began to conduct CoVPN work, along with sites in Latin America and sub-Saharan Africa.
During one early phone call, Karina Walters, co-director of the Indigenous Wellness Research Institute at the University of Washington, suggested that Andrasik and CoVPN establish panels of community experts. A panel of 10 to 15 scientists and community leaders was formed to review each of the vaccine protocols as well as community engagement plans for each of CoVPN’s focus populations: Native/Indigenous, Black/African American, Hispanic/Latino/a, and older adults/veterans. The panels’ input helped CoVPN craft inclusive recruitment materials from the beginning.
“It’s critical to have that input and that feedback early on so that you can show up in a respectful way and ensure that you are being inclusive, not only by your actions but your words,” says Andrasik. “You may not even know that you pushed someone away by using the wrong phrase or not understanding something.”

COVID-19 Prevention Network
This network was launched in July 2020 to test COVID-19 vaccines and other prevention tools.

The Bridge HIV outreach team in San Francisco promotes a study of broadly neutralizing antibodies. Photo courtesy of HIV Vaccine Trials Network.

The Bridge HIV outreach team in San Francisco promotes a study of broadly neutralizing antibodies. Photo courtesy of HIV Vaccine Trials Network.
Building trust and raising awareness
CoVPN staff also met regularly with members of NIH’s Community Engagement Alliance (CEAL) Against COVID-19 Disparities to discuss their community engagement successes and lessons learned. CEAL and CoVPN both worked with communities disproportionately affected by COVID-19. Although these communities were often in different locations, the two organizations saw similar patterns, says George Mensah, M.D., director of the Center for Translation Research and Implementation Science (CTRIS) at the National Heart, Lung, and Blood Institute (NHLBI) and a program leader of CEAL. A central finding was the importance of trust, truthfulness, and transparency.
“Ensuring that you are trustworthy overcomes almost everything,” says Mensah.
Building trust may look different in different communities. In Black and African American communities, Mensah says, he has found it most important to acknowledge past injustices and “make sure that people know that there are policies in place to protect research participants and that they can participate freely. They can also withdraw freely from the studies without any repercussions.”
American Indian communities also found it important to acknowledge past injustices but additionally sought legal protections to ensure the respectful and ethical use of data gathered from Tribal members during the vaccine clinical trials. David R. Wilson, Ph.D., director of the NIH Tribal Health Research Office, worked closely with many Tribal Nations that requested clear and accurate information on the development of COVID-19 vaccines. As a result, three Tribal Nations served by CoVPN sites worked with THRO, NIAID, and the vaccine sponsor to establish data sovereignty agreements that met each nation’s needs.
CoVPN also raised awareness of vaccine clinical trials through TV and digital media, including an advertisement with a voice-over by actor Harrison Ford and a blog series titled “COVID-19 Vaccine Matters.” Community advisory board members, local activists, and faith leaders provided vital on-the-ground outreach as trusted liaisons between clinical sites and the wider community.
In addition to building lines of communication and trust with communities, CoVPN sites sought to make it easier to participate in vaccine trials. The clinical sites were open during flexible hours, for example, so that participants with strict work schedules could get there. Sometimes the clinical sites could travel to the participants directly as mobile units.
Proof of what’s possible
When Andrasik and other colleagues from across CoVPN analyzed the data, they found that their efforts had paid off. Across four Phase 3 clinical trials, CoVPN sites worked with more than 130,000 volunteers, 47% of whom identified as BIPOC.
“We were hoping that our BIPOC numbers would at the very least represent the numbers in the larger U.S. population,” says Andrasik. “And the fact that we exceeded that just makes me happy every day.”
The CoVPN team looked closely at the data gathered during volunteer enrollment in the clinical trials to understand when different racial and ethnic groups enrolled. The results and analysis of CoVPN’s community engagement strategies, published in PLOS ONE in October 2021, showed that the strategies worked.
During the Phase 3 trial for the Moderna COVID-19 vaccine, which started enrolling participants before community engagement was underway, White people enrolled in much higher numbers earlier in the recruitment processes. To ensure diversity, sites running trials for that vaccine began to enroll only people of color.
Vaccine trials that started after CoVPN launched had higher enrollment from BIPOC communities from the start because of preexisting relationships and trust. The Novavax trial began last of the four COVID-19 vaccine trials conducted by CoVPN, and it was the only trial to start after CoVPN had established data sovereignty agreements with Tribal Nations. That had a clear impact on trial participation: While American Indian and Alaska Native individuals comprised about 2% of CoVPN vaccine trial populations on average, they were 6% of the Novavax trial population.
“It’s critical to have that input and that feedback early on so that you can show up in a respectful way and ensure that you are being inclusive, not only by your actions but your words.” —Michele Andrasik, Ph.D.
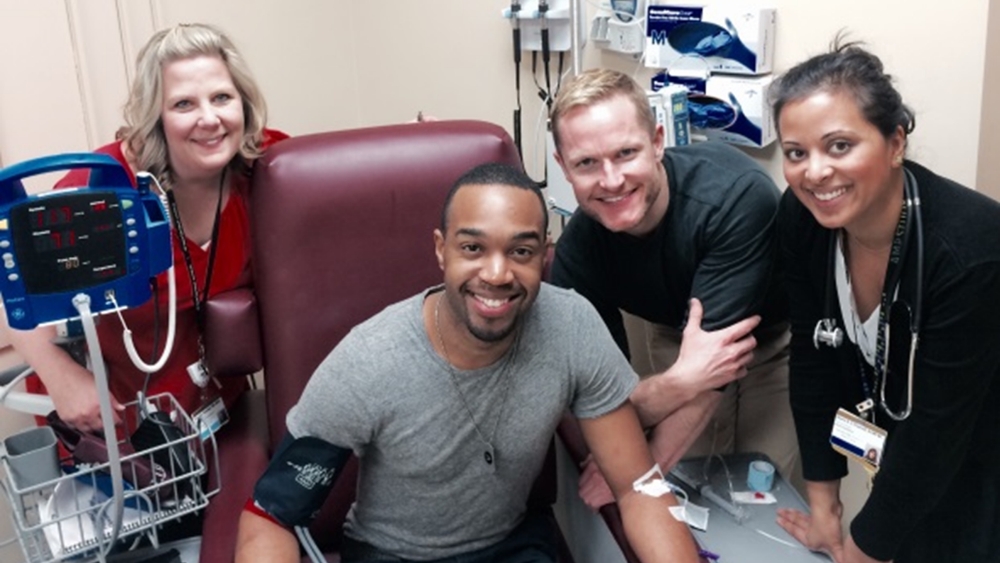
Clinic staff at Vanderbilt University in Nashville, Tennessee, pose with a participant during a study visit. Photo courtesy of HIV Vaccine Trials Network.

Clinic staff at Vanderbilt University in Nashville, Tennessee, pose with a participant during a study visit. Photo courtesy of HIV Vaccine Trials Network.
Engagement helps the community
For community engagement researchers, the CoVPN vaccine study participation numbers show the importance of involving communities in clinical trials from the beginning. COVID-19 has affected some communities more than others, and often the hardest-hit communities already experienced higher levels of other diseases.
“These disproportionate health impacts on communities existed before the pandemic, and they will be there after the pandemic,” says Mensah. He pointed particularly to heart disease, chronic lung disease, and sickle cell disease. “The process of developing interventions for all of these chronic diseases could benefit from many of the lessons we’ve learned through community engagement during the CoVPN COVID-19 vaccine trials.”
When clinical trials include people from communities most affected by the disease being studied, the trial results more accurately reflect how well the vaccine or medication will work in the real world. Having a diverse group of trial participants also builds trust in the trial’s results.
“One of the things that people ask us all the time is, ‘Who’s in the trial? Were there people that look like me in the trial?’” says Andrasik. “And it’s really great when the answer is that, yes, we recruited people who look like the whole United States population.”
Sources
- Andrasik, M. P., Broder, G. B., Wallace, S. E., Chaturvedi, R., Michael, N. L., Bock, S., Beyrer, C., Oseso, L., Aina, J., Lucas, J., Wilson, D. R., Kublin, J. G., & Mensah, G. A. (2021). Increasing Black, Indigenous and People of Color participation in clinical trials through community engagement and recruitment goal establishment. PLOS ONE, 16(10), e0258858. https://doi.org/10.1371/journal.pone.0258858
- Flores, L. E., Frontera, W. R., Andrasik, M. P., del Rio, C., Mondríguez-González, A., Price, S. A., Krantz, E. M., Pergam, S. A., & Silver, J. K. (2021). Assessment of the inclusion of racial/ethnic minority, female, and older individuals in vaccine clinical trials. JAMA Network Open, 4(2), e2037640. https://doi.org/10.1001/jamanetworkopen.2020.37640
- Haroz, E. E., Kemp, C. G., O’Keefe, V. M., Pocock, K., Wilson, D. R., Christensen, L., Walls, M., Barlow, A., & Hammitt, L. (2022). Nurturing innovation at the roots: The success of COVID-19 vaccination in American Indian and Alaska Native communities. American Journal of Public Health, 112(3), 383–387. https://doi.org/10.2105/AJPH.2021.306635
 An official website of the United States government
An official website of the United States government