Article Highlights
-
Wastewater testing offers anonymous, noninvasive tracking of SARS-CoV-2.
-
NIH is funding studies on the use of wastewater testing to monitor the virus at small geographical scales, such as universities, Tribal communities, and jails.
-
Wastewater testing could have value in future pandemics and disease outbreaks.
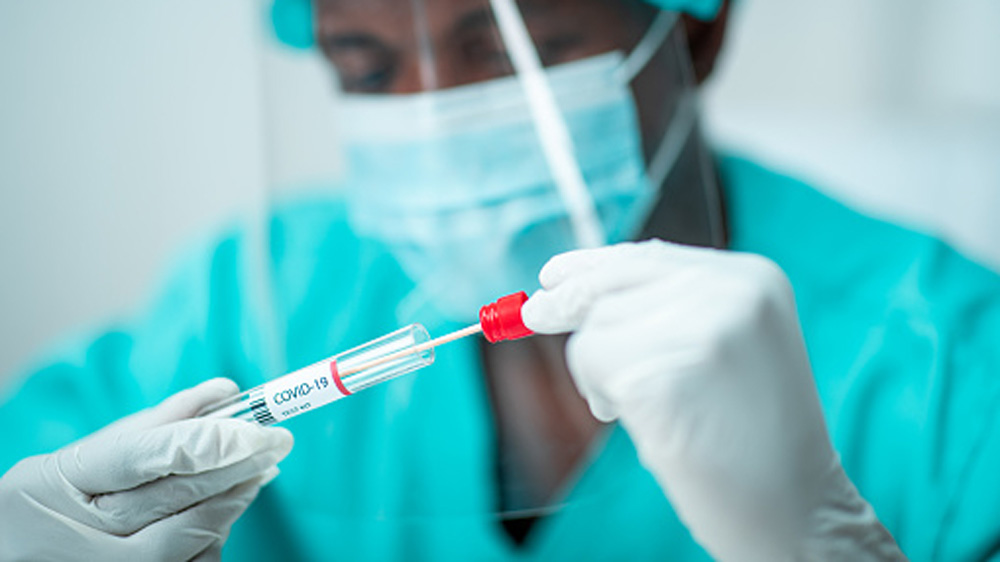
For one person, swabbing the nose is the best way to find out whether they have COVID-19. But for officials who need to track COVID-19 for a whole community, that approach to testing isn’t so easy.
Wastewater testing offers a way to monitor a community’s health without having to rely on testing individuals. In places with a sewer system, wastewater testing offers an unbiased view of whether SARS-CoV-2, the virus that causes COVID-19, is present; whether cases are going up or down; and even what variants are present. It’s also anonymous, since everyone’s wastewater is mixed together.
Helena Solo-Gabriele, Ph.D., PE, an environmental engineering researcher at the University of Miami in Coral Gables, Florida, has worked with her university to implement wastewater testing for the main campus and the university’s hospital. Some municipalities already test for SARS-CoV-2 at wastewater treatment plants. But that provides broad, citywide information, not highly localized data. People in different neighborhoods may have different risk factors, such as a higher probability of having to go to work in person, and people in institutions may live in close quarters.
In Dr. Solo-Gabriele’s studies and others funded by NIH, researchers are looking at wastewater testing on a smaller scale, such as in the wastewater from a single dormitory or in a smaller rural community, to get more detailed geographical information on outbreaks. The lessons learned from this research will help public health officials continue to monitor SARS-CoV-2 and get a better handle on disease outbreaks in the future.

Walter E. Lamar, Ph.D., executive director of Occupational Health, Safety and Compliance for the University of Miami Medical Campus, sets up an autosampler in a manhole on the University of Miami’s campus. Image courtesy of Matthew Roca.

Walter E. Lamar, Ph.D., executive director of Occupational Health, Safety and Compliance for the University of Miami Medical Campus, sets up an autosampler in a manhole on the University of Miami’s campus. Image courtesy of Matthew Roca.
Measuring SARS-CoV-2 in Miami
In the summer of 2020, the University of Miami’s leaders were planning for the fall semester. Students had the option to come back in person or virtually, but most faculty were encouraged to come back in person and to teach hybrid classes — and they wanted to know that they would be safe. “It was a very nerve-wracking period of time,” said Dr. Solo-Gabriele. “There was such a need, there was so much unknown, and everybody was nervous.”
Dr. Solo-Gabriele studies microorganisms in the environment, and she had heard about new research showing that SARS-CoV-2 could be found in wastewater. “It’s a good way to determine whether the community that was contributing to the wastewater was sick,” she said. “It didn’t matter if they were asymptomatic or symptomatic.” She wrote to the university’s president, who has a public health background, and offered to help. With his enthusiastic endorsement, and support from the university’s vice provost for research, who also has public health expertise, she got started, along with colleagues at the university’s medical school who were able to arrange to test the samples.
As her sampling was getting underway, Dr. Solo-Gabriele also applied for NIH funding through RADx® Radical (RADx-rad), a part of NIH’s Rapid Acceleration of Diagnostics (RADx®) initiative. RADx-rad is supporting nontraditional approaches that address gaps in COVID-19 testing. That includes support for wastewater analysis and other surveillance methods, particularly those focused on high-risk populations, to identify the virus and measure the spread of infection. She is working on this project, funded by RADx-rad and administered by the National Institute on Drug Abuse (NIDA), with Stephan Schürer, Ph.D., and George Grills of the University of Miami and Christopher Mason, Ph.D., of Weill Cornell Medicine in New York.
The team settled on sampling at seven residential dorms and at “clusters” — three manholes that allow access to sewage from the northern, central, and southern parts of campus before the wastewater enters the county’s system. They also had access to daily data on COVID-19 test results from each dorm, as well as the university’s testing on faculty and staff. “It was an awesome opportunity to collect data,” Dr. Solo-Gabriele said. The numbers the team saw from the sewage correlated closely with the university’s data from nasal swabs. “At the building level, it was like a light switch,” she said. When COVID-19 popped up at a building, administrators requested additional testing in that building, so infected students could be asked to isolate.
The team also tested wastewater at the university’s medical campus and at the facility where the campus’s sewage ultimately ends up, one of three wastewater treatment plants in Miami-Dade County. Results there showed peaks and valleys that aligned closely with hospitalization data and with data from the Florida Department of Health based on tests of individuals.
The team is also now collaborating on a RADx Underserved Populations (RADx-UP) project with local schools. In collaboration with Lisa Gwynn, D.O., M.B.A., M.S.P.H., of the University of Miami, Dr. Solo-Gabriele and her colleagues are sampling wastewater from elementary, middle, and high schools and comparing the SARS-CoV-2 levels with data on absenteeism. Wastewater testing could inform school officials about trends in COVID-19.
“Correctional health care is community health care. More than 90% of the people who are incarcerated at some point will return to the community. And we want to return people to the community healthy.” —Tracy Elam, Ed.D.
Monitoring wastewater in Tribal communities
Otakuye Conroy-Ben, Ph.D., (Oglala Lakota) is an environmental engineer at Arizona State University (ASU) in Tempe. Her project, also funded through RADx-rad and administered by NIDA, is implementing wastewater testing with Tribal communities across the country.
Wastewater testing can be difficult in Tribal communities, because many are in remote areas with low sewer flows. Doing research in Tribal communities can also be complex. “There’s been a lot of mistrust between academic institutions and Tribal Nations when it comes to research,” Dr. Conroy-Ben said. Research with Tribes also requires a Tribal Consultation process in which NIH and the Tribe discuss the proposed research and how it would affect the Tribe.
The first step in testing wastewater on Tribal land is finding out where it is even a possibility. Of 574 federally recognized Tribes, about 325 have Tribal land, and of those, only a little more than 100 have permits from the Environmental Protection Agency (EPA) that allow them to treat wastewater to the point where it can be discharged into waterways. Those Tribes might have enough treatment infrastructure to consider wastewater testing. (Other Tribes handle wastewater in other ways, such as septic systems.)
Dr. Conroy-Ben got started studying wastewater with a pilot project with one Tribe in 2016 and 2017. In that project, Dr. Conroy-Ben and her colleagues were able to measure opioids, other illicit drugs, and medications in the wastewater — and showed that it is possible to use wastewater testing to study health in remote rural communities. The team continued building relationships with Tribes in hopes of doing more research along those lines.
When the pandemic started, the researchers contacted the Tribes about wastewater testing for SARS-CoV-2. With support from the National Science Foundation, the researchers carried out a pilot project with one Tribe. Later, the team received funding through NIH’s RADx-rad program. Dr. Conroy-Ben focuses on relationships with Tribes, and she is collaborating with ASU’s Rolf Halden, Ph.D., M.S., who tests the samples, and Kerry Hamilton, Ph.D., M.H.S., who focuses on sampling methods and the risks of sampling wastewater.
Although Tribes with wastewater infrastructure have to sample the water that comes out of the treatment process to ensure they are satisfying EPA requirements, they do not necessarily have anyone sampling sewage before it is treated. When a new Tribal partner agrees to participate in the research, Dr. Conroy-Ben travels to the Tribe’s location to examine the infrastructure and decide where to sample. Her goal is to find a manhole with access to untreated sewage. The research team collects the sewage using an automatic sampler that samples every hour for 24 hours.
The team is sampling each Tribe’s wastewater only once a month, which does not provide enough data to Tribes to make public health decisions. However, Dr. Conroy-Ben hopes that the groundwork she has done will offer a template that any Tribe with wastewater treatment can use to monitor COVID-19 on their own.

RADx-rad Wastewater Awardees
RADx-rad funded seven projects on detecting SARS-CoV-2 in wastewater in a variety of settings.

Members of the Emory University project team collect wastewater from a manhole outside the Fulton County Jail. Image courtesy of Anne Spaulding.

Members of the Emory University project team collect wastewater from a manhole outside the Fulton County Jail. Image courtesy of Anne Spaulding.
Tracking COVID-19 in a county jail
Jails and prisons have particularly struggled in the COVID-19 pandemic, with many people living in close quarters. Starting in the summer of 2021, Fulton County Jail in Atlanta has partnered with a public health team at Emory University led by physician and epidemiologist Anne Spaulding, M.D., M.P.H., to expand the jail’s testing strategy. Dr. Spaulding worked with the Fulton County Sheriff’s Office to roll out mass testing with self-swabbing; up until then, jail health care workers had tested residents of the jail.
Although effective, swabbing individual noses is expensive and requires extra staff, such as an accompanying correctional officer, to keep it going. The jail needed a more efficient way to watch for COVID-19. Starting in mid-2021, a team headed by Dr. Spaulding and Emory colleague Christine Moe, Ph.D., piloted wastewater testing, with support from the RADx Tech initiative. The team identified four manholes where they could collect sewage samples for weekly monitoring. The manholes give access to sewage from the jail’s north and south towers, where people stay while they are awaiting trial, and also from the jail’s infirmary.
Because they tested the wastewater at the same time as they ran mass testing within the jail population, the team could compare the amount of SARS-CoV-2 detected in sewage against the number of cases identified with swabs. From December 2021 through January 2022, both the swab and wastewater data captured a large spike in COVID-19 cases. “We have a clear demonstration that this technology works in a jail,” Dr. Spaulding said.
The team plans to continue COVID-19 wastewater testing at Fulton County Jail through the spring of 2023. They are also conducting a demonstration of wastewater testing in a handful of prisons in Alabama. If they can replicate their results in Alabama, the team will work to implement wastewater testing long-term in the Fulton County Jail. Through a project supported by RADx-UP and administered by NIDA, Dr. Spaulding and her team are also working with other researchers to establish and sustain wastewater testing protocols at local jails in Chicago; Washington, D.C.; and Middlesex County, Massachusetts.
“I have tremendous respect for Dr. Anne Spaulding and her vision,” said Fulton County Sheriff Patrick Labat. “Dr. Spaulding’s unique, analytical approach to tracking the coronavirus will not only benefit the jail population and surrounding areas but also aid other scientists in tracking the patterns of the virus and saving lives.”
Dr. Spaulding expects wastewater testing to be easier to maintain over an extended time than swabbing individual noses, with less requirement for increased staffing or individual participation. If wastewater samples show that there is more virus in the wastewater, then jail health care workers can begin asking individuals to swab their noses for COVID-19 testing — and can save trouble by focusing on specific towers or housing blocks.
Through this partnership between Emory University and Fulton County Jail, the team hopes to protect the health of both incarcerated people and the wider community amid the long-term prospect of widespread COVID-19.
“Correctional health care is community health care,” said Tracy Elam, Ed.D., Fulton County Jail’s health program manager. “More than 90% of the people who are incarcerated at some point will return to the community. And we want to return people to the community healthy.”
Wastewater testing into the future
Research projects like these, and the methods for collecting wastewater testing data that are being developed along with them, will help public health officials and leaders of institutions monitor COVID-19 in the long term and on a variety of scales.
And it doesn’t stop with COVID-19. Dr. Solo-Gabriele’s testing with Miami-Dade County schools has inspired thoughts of tracking other diseases that can be dangerous for children, such as respiratory syncytial virus (RSV), flu, or severe diarrheal conditions. “The school could send families the information that something is going around, instead of just waiting until everybody gets sick,” Dr. Solo-Gabriele said. For example, if RSV were on the rise, principals could suggest masks or take other steps to keep children safe. Her team has also sampled wastewater from the University of Miami’s hospital. Among other things, they have tested for Candida auris, a fungus that can cause serious problems in health care settings. If wastewater testing proves to be an effective way to identify C. auris outbreaks, it could help hospitals in the future.
“Now we know that we can do this to track infectious disease. In addition to SARS-CoV-2, what else can we look for?” Dr. Solo-Gabriele said.
 An official website of the United States government
An official website of the United States government