Article Highlights
-
Tests can identify infection pockets and when people should isolate to avoid passing on the virus.
-
The White Mountain Apache Tribe and Navajo Nation are participating in a study on testing.
-
The study explores two different ways of encouraging people to get COVID-19 tests.
When COVID-19 reached the White Mountain Apache Tribe in the spring of 2020, Francene Larzelere and her colleagues sprang into action. Larzelere, an enrolled member of the tribe, helps run several behavioral health projects at the Johns Hopkins Center for American Indian Health in Whiteriver, Arizona.
Larzelere and her colleagues began calling people who had tested positive for COVID-19 to check on them, share information about the pandemic in English and Apache, and even deliver boxes of food to households that were quarantined. “It helped to assure people that there was support; if they needed something, they could call us,” she said.
Now Larzelere and her colleagues are beginning a research study on how to reduce transmission of the virus. The team will try out two different ways to encourage more people to get tested as soon as possible after exposure. Testing soon after symptoms appear is an important part of controlling outbreaks of COVID-19. Both the White Mountain Apache Tribe and the Navajo Nation are participating in the research study, which is part of the Rapid Acceleration of Diagnostics-Underserved Populations (RADxSM-UP) program, which is working to increase COVID-19 testing for underserved and vulnerable populations across the United States.
"Fast, accurate, reliable testing for COVID-19 should help everyone return to normal life sooner. Tests help identify pockets of infection and make it clear if specific people should isolate, so they can avoid passing the virus on to anyone else."

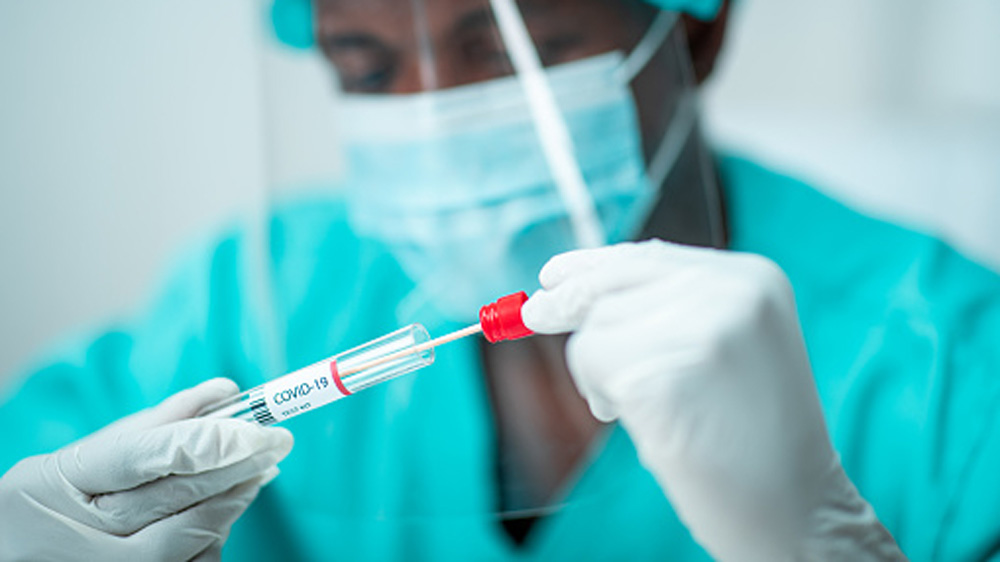
Dr. Diana Hu administers a COVID-19 test during a testing blitz on the Navajo Nation.
Credit: Dr. Nina Mayer Ritchie

Dr. Diana Hu administers a COVID-19 test during a testing blitz on the Navajo Nation.
Credit: Dr. Nina Mayer Ritchie
Turning to Testing
“What we are trying to do — our overall goal — is to really increase testing,” said Mary Cwik, Ph.D., one of the study’s leaders and an associate director of the Johns Hopkins Center for American Indian Health. She is based at the Center’s administrative headquarters in Baltimore, Maryland.
Fast, accurate, reliable testing for COVID-19 should help everyone return to normal life sooner. Tests help identify pockets of infection and make it clear whether specific people should isolate, so they can avoid passing the virus on to anyone else.
Researchers at the Center for American Indian Health choose research directions based on community guidance. Cwik, a child psychologist, usually focuses on youth suicide prevention, a major concern for tribal leaders. She has worked with the White Mountain Apache Tribe for more than a decade and, more recently, with the Navajo Nation as well.
When the community’s needs change, as they did at the beginning of the pandemic, so does the research. “Obviously, when all of this hit, that was what was on the community’s mind,” Cwik said. “We try to be responsive in whatever way we can to their needs.”
Cwik and her colleagues applied for funding through RADx-UP to help address the community’s concerns about the pandemic. Their study on COVID-19 testing is funded through the NIH Office of the Director, while Cwik’s suicide prevention research is funded through the National Institute of Mental Health (NIMH).
The Old and the Young
The study will recruit participants from two groups: elders age 65 and up and young adults ages 18 to 34.
Older people are at high risk of serious complications and even of dying from COVID-19. They may also have beliefs that stand in the way of getting testing, Cwik said. For example, elders may fear that testing positive could lead to being taken away from their home and family, to receive specialty medical care off the reservation. Elders might also be hesitant to trust government health services because of negative past experiences.
Young adults seem to be particularly prone to spreading the virus, because many have continued socializing, Larzelere said. Another reason for focusing on young people is that they have the highest risk for substance use problems — which can lead to being close together with friends, sharing containers, or other behaviors that raise the risk of spreading the virus, she said. In addition, many young adults of the White Mountain Apache Tribe and Navajo Nation live with older relatives who are at high risk.

Featured Resource
NIMH's COVID Resources
Explore resources from NIMH about coping with the stress of the COVID-19 pandemic.
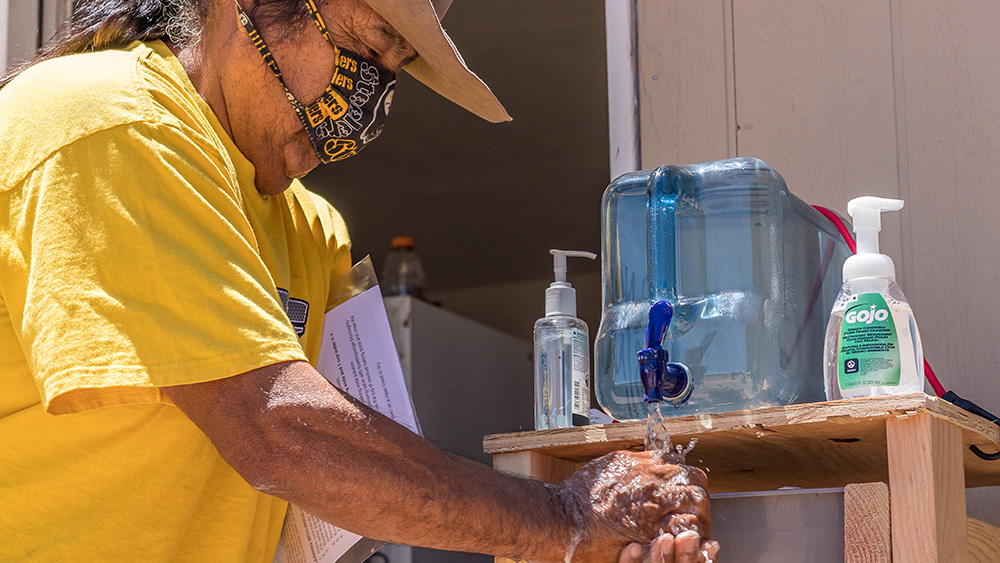
A Navajo elder washes his hands with a newly built handwashing station.
Credit: Dr. Nina Mayer Ritchie
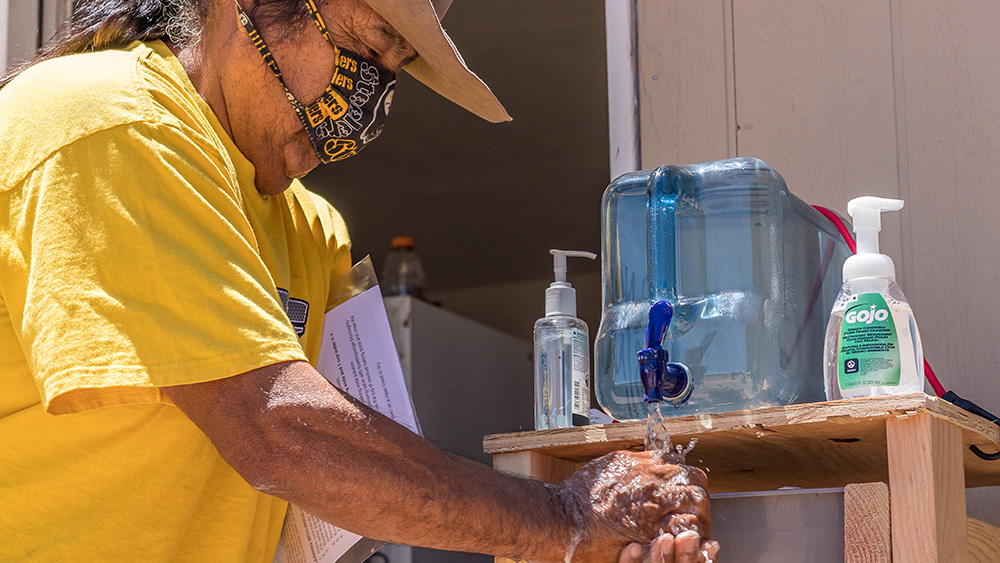
A Navajo elder washes his hands with a newly built handwashing station.
Credit: Dr. Nina Mayer Ritchie
Testing Different Approaches
The team is exploring two different ways of encouraging people to get COVID-19 testing. One is a monitoring system that automatically texts each person once a day to ask a few questions about their symptoms and their exposure. People in that group will also be given a thermometer and a pulse oximeter, a tool that measures how much oxygen is in the blood. If the answers suggest that they should be tested, a case manager will call and text them to offer a home test or transportation to a testing site.
The other is motivational interviewing, a way to help gently nudge people to think about taking actions that they might feel reluctant about. In the case of COVID-19, people might be reluctant to take actions such as testing, wearing a mask, and quarantining after exposure. A family health coach will interview each person two or three times, regardless of whether they have symptoms. In the interview, the coach and participant will discuss reasons for avoiding testing — such as fear of having to stay home from work — and reasons to get testing, such as helping protect family members from disease. Other studies have found that motivational interviewing can reduce substance misuse and increase testing for HIV and sexually transmitted diseases.
People who sign up for the study will be randomly assigned to one of four groups: daily texting, motivational interviewing, both of those, or neither. Everyone in the study will receive basic information about COVID-19 and hygiene kits containing items such as masks and cleaning products.
Getting Started
The team hopes to start signing up participants for the study in February. Researchers will follow each participant for three months and measure how long it takes for them to get a COVID-19 test after exposure or developing symptoms. The team will also track how many people in each group are choosing to get tested.
Once they have determined whether texting or motivational interviewing helps encourage people to get tested quickly, the researchers will share their findings with others who might be able to adapt the approach for their own communities.
“I think this project is going to expand what we are able to do and reach more people — to slow the spread and bring more awareness to people,” Larzelere said.
 An official website of the United States government
An official website of the United States government