Article Highlights
-
Learn about the NIH’s Vaccine Research Center from Director John Mascola, M.D.
-
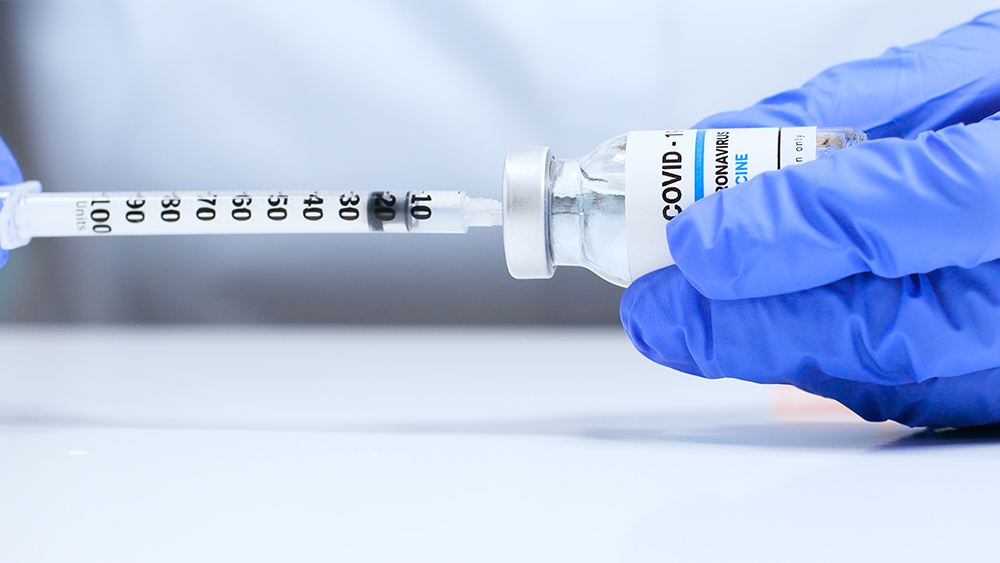
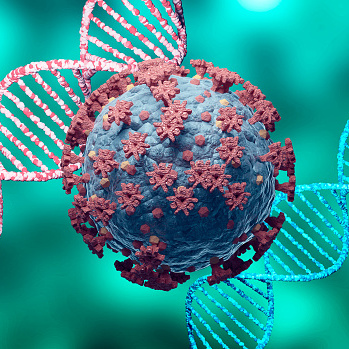
Vaccines save lives and can help stop the spread of SARS-CoV-2 and its variants.
-
Decades of VRC research led to rapid development of the Moderna mRNA vaccine.
The Moderna vaccine for COVID-19 may seem like it developed quickly, but it was built on decades of research by NIH’s Dale and Betty Bumpers Vaccine Research Center (VRC). The scientists of the VRC have learned from experience by studying the immune system and working on vaccines for other infectious diseases that pose major threats to human health around the world.
The U.S. Food and Drug Administration has authorized three vaccines to prevent COVID-19. Two of them are based on messenger RNA (mRNA) technology. One of the mRNA vaccines — the Moderna vaccine — resulted from VRC scientists’ work with researchers from the Moderna company and other organizations.
Both the Moderna and Pfizer mRNA vaccines are more than 90% effective at preventing infection with SARS-CoV-2, the virus that causes COVID-19. As of June 18, 2021, more than 300 million doses of mRNA vaccines have been given in the United States.
John Mascola, M.D., is the director of the VRC, which is part of the National Institute of Allergy and Infectious Diseases (NIAID), one of NIH’s 27 Institutes and Centers. VRC scientists work on safe and effective vaccines for human disease.
Mascola spoke with us about his career, what it takes to conquer a pandemic, and the research “building blocks” that led to COVID-19 vaccine success.

John Mascola, M.D., was one of the VRC’s founding investigators. He now serves as the center’s Scientific Director and Center Director. Photo credit: NIAID, NIH.

John Mascola, M.D., was one of the VRC’s founding investigators. He now serves as the center’s Scientific Director and Center Director. Photo credit: NIAID, NIH.
NIH: How does it feel to know millions of people around the world are getting a vaccine that resulted from your work?
Mascola: Realizing that our work is having a worldwide impact, saving many thousands of lives, is pretty amazing. It’s been exciting and rewarding to see how decades of hard work by NIH scientists and the foresight of public health leaders have come together to develop vaccines to control the pandemic.
NIH: What is the VRC? How did it come about?
Mascola: The idea behind the VRC came from discussions at NIH back in 1996 about unifying all of NIH’s work on vaccines for HIV/AIDS. Construction of the center was complete in 2000.
The VRC is home to scientists with expertise in all aspects of vaccine development, starting with basic science and structural biology, through clinical trials, and even vaccine production. We work with scientists in universities, other agencies, and pharmaceutical and biotechnology companies. The VRC’s organizational structure has been very productive.
NIH: Tell us a bit about your personal and professional journey to becoming the head of the VRC.
Mascola: I started out as an infectious disease doctor. I began to focus on how the human immune system works — and how it doesn’t work in certain health conditions, especially HIV/AIDS. My research on immunity and HIV grew into an interest in vaccines. Working on vaccines to prevent HIV/AIDS at the VRC was a natural fit for me.
“It may seem like the COVID-19 vaccines were made in a hurry, but it’s actually been decades of work.” —John Mascola, M.D.
NIH: Why haven’t we been able to develop a vaccine for HIV/AIDS?
Mascola: There’s been some progress in developing a vaccine against HIV, but HIV is very challenging. The virus’s genetic code mutates (changes) often, and the virus has unique ways of evading the immune system.
But the investment in HIV science over the past two decades has helped fight other diseases. HIV vaccine studies have taught us much about how the human immune system works and about vaccines. Those discoveries and insights are the scientific building blocks that made it possible to create safe and effective vaccines against COVID-19 in a short time. It may seem like the COVID-19 vaccines were made in a hurry, but it’s actually been decades of work.
NIH: How does COVID-19 vaccine development build upon the VRC’s earlier work?
Mascola: We’d learned that mRNA vaccines stimulate strong immune responses in the body. The vaccines can be produced in a few weeks because you don’t have to grow the virus in the lab. You just need to know the virus’s genetic code to design a vaccine.
The VRC has been collaborating with Moderna since 2015 on vaccines for HIV and Zika virus. More recently, we had been working on a demonstration project for rapid production and clinical testing of mRNA vaccines. In addition, VRC scientists have been studying other coronavirus diseases.
So, when we heard reports about an outbreak of COVID-19 in early 2020, the VRC and Moderna were ready to take action to create an mRNA vaccine to prevent COVID-19. The result was the Moderna mRNA vaccine that’s saving millions of lives.
NIH: Am I safe if I got vaccinated?
Mascola: You are much, much safer than people who aren’t vaccinated.
All the authorized vaccines provide very good protection from getting COVID-19, and if you do get it, you are far less likely to have severe disease that requires hospitalization, an ICU stay, or ventilator support.
People can be confident that the vaccines are safe. The vaccines have gone through every step of safety testing. The FDA reviews all data before authorizing vaccines.
I rolled up my sleeve for a vaccination on the first day I was eligible, and I encouraged my family and friends to do the same. Getting vaccinated gives you a personal sense of freedom.
Like all vaccines, COVID-19 vaccines can have some expected, manageable side effects, including pain at the injection site, muscle soreness, and headache. More serious side effects, like blood clots, are extremely rare.
It’s clear that the benefits of the vaccines far outweigh the risks of COVID-19.

The Story Behind COVID-19 Vaccines
NIAID Director Anthony Fauci, M.D., explains how decades of research by VRC scientists and others contributed to the rapid development of COVID-19 vaccines.

Home of the Dale and Betty Bumpers Vaccine Research Center on the main campus of NIH in Bethesda, Maryland. Source: National Cancer Institute Visuals Online.

Home of the Dale and Betty Bumpers Vaccine Research Center on the main campus of NIH in Bethesda, Maryland. Source: National Cancer Institute Visuals Online.
NIH: What else is going on at the VRC?
Mascola: Even as we work on COVID-19 vaccines, we have kept our other programs active.
The VRC is working on vaccines for other viral diseases, including Ebola virus and Zika virus diseases, as well as diseases caused by bacteria, such as tuberculosis. We also work on parasitic diseases like malaria.
For influenza (flu), VRC scientists are testing universal vaccines. A universal vaccine would work against more strains of flu and give longer-lasting immunity than the current vaccines. Imagine if you only needed one flu shot and maybe a couple of booster doses throughout your lifetime instead of having to get a shot every year.
NIH: What keeps you up at night?
Mascola: Whatever the latest COVID-19 emergency is.
Right now, I worry about new variants (strains) of SARS-CoV-2. The more the virus multiplies, the more chances it has to mutate and become a variant of concern. Variants of concern may spread more quickly, cause more severe disease, or be resistant to vaccines and treatments.
So far, our vaccines seem to provide protection against variants, but we need to take steps, like increasing vaccination rates, to stop the virus from multiplying.
NIH: How can we better prepare for public health emergencies like the COVID-19 pandemic?
Mascola: We recognize on all levels — political, scientific, and individual — that pandemics can happen anytime, anywhere. COVID-19 is the third coronavirus outbreak in less than 20 years. You don’t need a crystal ball to know that more outbreaks are likely.
We need a better understanding of major virus “families” that affect humans, plus a stronger global surveillance system to watch for new microbes with the potential to cause human disease.
Finally, we have to set up rapid-response plans so we can quickly design and produce vaccines when new diseases pop up. We need to have enough manufacturing facilities to produce large numbers of doses.
We were able to rapidly create a vaccine in response to the COVID-19 pandemic because of the years spent in building a knowledge base about coronaviruses and mRNA vaccines. This was only possible through research investments in virology, immunology, and vaccines by NIH and other parts of the public sector, together with vaccine research and development in the private sector.
Sources
- Collins, F. (2021). A Real-World Look at COVID-19 Vaccines Versus New Variants. NIH Director’s Blog. Retrieved May 3, 2021, from https://directorsblog.nih.gov/2021/05/04/a-real-world-look-at-covid-19-vaccines-versus-new-variants/.
- Corey, L., Mascola, J. R., Fauci, A. S., & Collins, F. S. (2020). A strategic approach to COVID-19 vaccine R&D. Science (New York, N.Y.), 368(6494), 948–950. https://doi.org/10.1126/science.abc5312.
- Global Change Data Lab. (2021). Our World in Data. COVID-19 Vaccine Doses Administered, by Manufacturer, in the United States. Retrieved May 17, 2021, from https://ourworldindata.org/grapher/covid-vaccine-doses-by-manufacturer.
- Mascola, J. R., & Fauci, A. S. (2020). Novel vaccine technologies for the 21st century. Nature Reviews. Immunology, 20(2), 87–88. https://doi.org/10.1038/s41577-019-0243-3.
- Thompson, M. G., Burgess, J. L., Naleway, A. L., Tyner, H. L., Yoon, S. K., Meece, J., … Gaglani, M. (2021). Interim estimates of vaccine effectiveness of BNT162b2 and mRNA-1273 COVID-19 vaccines in preventing SARS-CoV-2 infection among health care personnel, first responders, and other essential and frontline workers — Eight U.S. locations, December 2020–March 2021. MMWR. Morbidity and Mortality Weekly Report, 70(13), 495–500. https://doi.org/10.15585/mmwr.mm7013e3.
- U.S. Food and Drug Administration. (2021). COVID-19 Vaccines. Retrieved May 11, 2021, from https://www.fda.gov/emergency-preparedness-and-response/coronavirus-disease-2019-covid-19/covid-19-vaccines.
 An official website of the United States government
An official website of the United States government